Trends in the Palliative Surgical Management of Patients With Unresectable Pancreatic Adenocarcinoma: Lessons Learned From a Large, Single Institution Experience
Peter J. Kneuertz*, Steven Cunningham, Sergio Lopez, John L. Cameron, Joseph M. Herman, Martin a. Makary, Frederic E. Eckhauser, Kenzo Hirose, Barish H. Edil, Michael a. Choti, Richard D. Schulick, Christopher L. Wolfgang, Timothy M. Pawlik
Department of Surgery, The Johns Hopkins University School of Medicine, Baltimore, MD
Introduction: Traditionally, routine palliative bypass (PBP) has been advocated for palliation of patients (pts) with pancreatic adenocarcinoma (PAC) who are explored with curative intent but have inoperable disease discovered at the time of surgery. We examined trends in the relative use of PBP over time with a particular emphasis on identifying changes in surgical indications, type of bypass performed, as well as perioperative outcomes associated with surgical palliation. Methods: Between Jan 1996 and Jun 2010, 1913 pts with PAC in the head of the pancreas were surgically explored. Data regarding preoperative symptoms, intraoperative findings, type of surgical procedure performed, as well as perioperative and long-term outcomes were collected and analyzed using univariate and multivariate analyses.Results: Of the 1913 pts, 1330 (70%) underwent a pancreaticoduodenectomy, while 583 (30%) did not. Among the 583 pts who did not undergo curative intent surgery, most presented with either preoperative nausea/vomiting (18%) or jaundice (72%). The majority of pts had been evaluated by CT scan (97%), while a minority had an MRI (5%) or PET scan (1%). On preoperative imaging, median size of the pancreatic lesion was 3.2cm with a median CA19-9 of 351 ng/dl. At surgery, 553 (95%) pts had PBP and 30 (5%) patients had laparotomy+biopsy without further surgical intervention. Among the 553 pts who had PBP, most (65%) underwent double bypass, while a minority had either gastrojejunostomy (28%) or hepaticojejunostomy (7%) alone. While the number of pancreaticoduodenectomies remained relatively stable over time, there was a temporal decrease in the utilization of PBP (Figure). Unanticipated locally advanced disease vs. liver/peritoneal metastasis as the indication for PBP also changed over time (1996-2001: 46% vs. 54%; 2002-2007: 49% vs. 51%; 2008-2010: 20% vs. 80%, respectively)(P=0.009). Following PBP, median length of stay was 8 d and 37% pts had a complication (major: 14%) with a readmission rate of 18%. Postoperative mortality after PBP was 2%. Few pts developed late obstruction (enteric: 3%; biliary: 4%) or needed a postoperative stent (enteric: 2%; biliary:5%). Overall survival following PBP was 6 months; pts with unsuspected metastatic disease as the indication for PBP had a significantly worse survival compared with pts who had locally unresectable disease (median survival: 5 vs. 8 months, respectively; HR=1.43, P=0.001). Conclusion: Utilization of PBP for inoperable pancreatic cancer has significantly decreased over time. The indication for PBP has also changed over time, with the discovery of unsuspected metastatic disease now being the main indication for PBP. While PBP remains effective, the morbidity can be significant and survival following PBP especially among pts with metastatic disease is extremely short.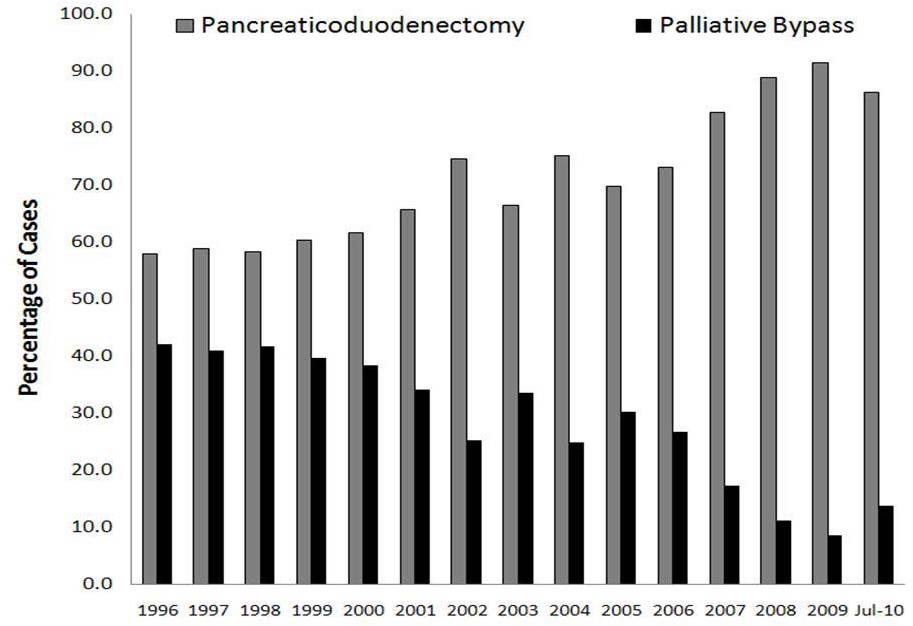
Back to 2011 Program



