Incidence and Impact of a Close Superior Mesenteric Artery Margin Following Pancreaticoduodenectomy for Adenocarcinoma
Matthew Katz*1, Huamin Wang2, Aparna Balachandran3, Priya Bhosale3, Xuemei Wang4, Peter W. T. Pisters1, Jeffrey E. Lee1, Doug B. Evans5, Chusilp Charnsangavej3, Jason B. Fleming1
1Surgical Oncology, UT MD Anderson Cancer Center, Houston, TX; 2Pathology, UT MD Anderson Cancer Center, Houston, TX; 3Diagnostic Radiology, UT MD Anderson Cancer Center, Houston, TX; 4Biostatistics, UT MD Anderson Cancer Center, Houston, TX; 5Surgery, The Medical College of Wisconsin, Milwaukee, TX
Background: The margin most commonly positive following pancreaticoduodenectomy lies adjacent to the superior mesenteric artery (SMA). In patients with rectal cancer, tumor cells within 1mm of the analogous radial margin predict early treatment failure. The significance of cancer within 1mm of the SMA margin in patients with pancreatic cancer is unknown. A recent analysis of national practice patterns documented a lack of attention to the SMA dissection (Katz MHG, Ann Surg Onc 2010, PMID: 20811779). We therefore sought to determine the incidence and significance of a close SMA margin. Methods: All 194 patients with pancreatic adenocarcinoma who underwent pancreaticoduodenectomy between 2004 and 2008 were evaluated. The SMA margin dissection was performed directly along the periadventitial plane of the SMA in all cases. The distance between cancer and the SMA margin was measured and prospectively recorded using a standard histopathologic protocol. The corresponding distance between tumor and the SMA was retrospectively measured on the preoperative computed tomogram. The concordance correlation coefficient between these measures was calculated.Results: A positive SMA margin was identified in 8 (4%) specimens. Accurate histologic measurements were available in 178 (96%) of 186 patients with a negative SMA margin; of these, the free margin measured ≤ 1mm in 40 (22%) patients, between 1 and 10mm in 72 (40%), and ≥ 10mm in 66 (37%). Neoadjuvant chemotherapy and/or chemoradiation was delivered to 150 (77%) patients; a positive SMA margin was identified in 3 (2%) of these patients versus 5 (11%) of the 44 patients who received no preoperative therapy (p = 0.02). Locoregional recurrence developed in 23% of patients with a negative SMA margin ≤ 1mm and 21% of patients with a negative margin > 1mm (p= 0.84). The overall survival of patients with a negative SMA margin ≤ 1mm did not differ from that of patients with a negative margin > 1mm (median 33 [95% CI: 22, 44] months v. 38 [95% CI: 34, 43] months, p = 0.12). Preoperative CT predicted a negative SMA margin (median 8.5mm, range 3 - 18mm) in 6 (75%) of 8 patients in whom it was positive. The concordance coefficient between the pathologic (median 2mm) and radiographic (median 8mm) measurements of the SMA margin in patients with a margin < 10mm was 0.07 (95% CI: 0.02, 0.13) (Figure).Conclusions: Despite the use of neoadjuvant therapy and a standardized approach to SMA dissection, the SMA margin was positive or measured ≤ 1mm in 26% of specimens following resection for adenocarcinoma of the pancreatic head. The proximity of cancer cells to the SMA was routinely underestimated by standard preoperative imaging. Nonetheless, associated with optimal surgical technique and the routine use of multimodality therapy, microscopic cancer approximating the SMA did not have a significant impact upon survival.
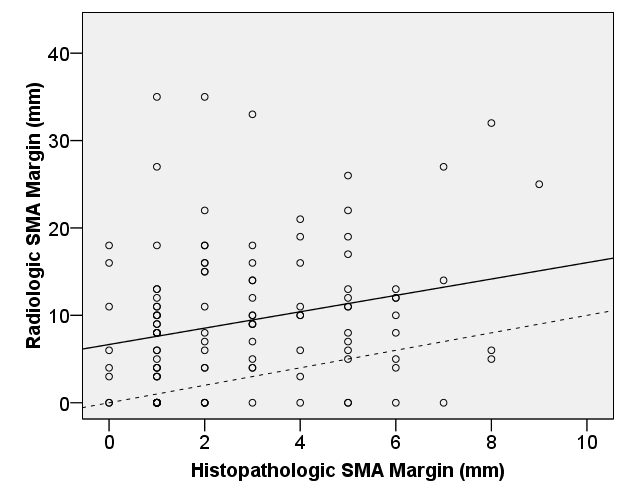
Correlation between SMA margin measured on preoperative CT scan and upon histopathologic evaluation
Back to 2011 Program



