RT-PCR Increases Detection of Submicroscopic Peritoneal Metastases in Gastric Cancer and Has Prognostic Significance
Joyce Wong*, Kaitlyn J. Kelly, Arjun Mittra, Mithat Gonen, Peter J. Allen, Yuman Fong, Daniel G. Coit
Surgery, Memorial Sloan-Kettering Cancer Center, New York, NY
Background: Positive peritoneal cytology confers the same prognosis as stage IV disease in gastric cancer. Conventional cytology, however, has low sensitivity. We propose that RT-PCR may have increased sensitivity and provide more accurate staging information.Methods: From 2/2007 to 4/2009, peritoneal lavage samples were collected prospectively from 156 patients with biopsy proven gastric cancer undergoing staging laparoscopy. These washings were analyzed by both Papanicolaou staining and real-time polymerase chain reaction (RT-PCR) for the tumor marker carcinoembryonic antigen (CEA). Results: Peritoneal disease was discovered at laparoscopy in 38 of the 156 patients (24%), (LAP+). Cytology was positive (CYT+) in 23 of these patients while RT-PCR was positive (PCR+) in 30. The sensitivity of CYT for detection of disease was 61% vs. 79% for PCR (p=.02). Non-stage IV disease was identified at laparoscopy in 118(76%) patients. Eight(7%) were CYT+ while 28(24%) were PCR+. Long term follow-up demonstrated worse survival of PCR+CYT- (p=.0003) and PCR+CYT+ (p=.0004) compared to CYT-PCR- patients. Resection was performed in 98 of these patients. A significantly greater proportion of patients with advanced stage disease, poor pathologic features such as vascular or perineural invasion, or who recurred after resection were PCR+ as compared to CYT+.An R0 resection was performed in 85(87%) patients: only one(1%) was CYT+ while 13(15%) were PCR+. Of this group, PCR+ demonstrated a worse survival than PCR- patients(p=.02). (Figure 1A). Further analysis showed that of the stage III/IV, CYT- subgroup, PCR+ had a trend towards worse survival (p=.09) than PCR- patients (Figure 1B).Conclusion: RT-PCR for CEA increases detection of submicroscopic peritoneal disease and is more sensitive than cytology. PCR positivity was associated with decreased survival. Further followup is required to determine if PCR can be used as an independent predictor of poor survival in gastric cancer.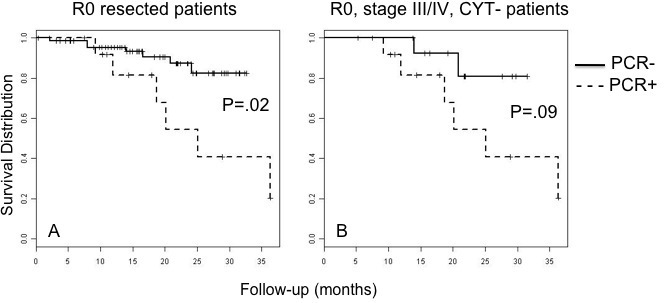
Survival distribution curves of R0 resected patients (A) and R0, stage III/IV, cytology negative patients (B) by PCR status. In patients who underwent R0 resection, PCR+ patients had a significantly worse survival than PCR- patients (p=.02). In the R0 resected, stage III/IV, cytology negative patients, PCR+ had a trend towards worse survival than PCR- patients (p=.09).
Back to 2011 Program



