THE LAPAROSCOPIC HELLER-DOR IS AN EFFECTIVE LONG-TERM TREATMENT FOR END-STAGE ACHALASIA
Giulia Nezi*, Francesca Forattini, Federica Riccio, Arianna Vittori, Luca Provenzano, Giovanni Capovilla, Loredana Nicoletti, Lucia Moletta, Elisa Sefora Pierobon, Gianpietro Zanchettin, Michele Valmasoni, Stefano Merigliano, Mario Costantini, Renato Salvador
Universita degli Studi di Padova, Padova, Veneto, Italy
BACKGROUND: Laparoscopic Heller-Dor (LHD) is an effective treatment for esophageal achalasia, with good long-term results in more than 85-90% of patients. It remains controversial whether LHD is also indicated in the end-stage disease when the esophagus has a sigmoid shape.
The aim of this study was to evaluate the outcome of LHD in patients with end-stage achalasia, as compared to patients with megaesophagus but without a sigmoid shape.
METHODS: From 1992 to 2020, patients with a radiological diagnosis of sigmoid-shaped esophagus (radiological stage IV achalasia: group SE) and patients with straight, larger than 6 cm in diameter esophagus (radiological stage III achalasia: group NSE), both treated with LHD, were compared.
Symptoms were scored using the Eckardt score. Barium-swallow, endoscopy and High Resolution or Conventional Manometry were performed before and after the treatment. Treatment failure was defined as the persistence or reoccurrence of an Eckardt score > 3, or the need for retreatment.
RESULTS: During the study period, 164 such patients were observed: 73 patients in the SE group and 91 in the NSE group. The patients' demographic and clinical parameters are summarised in table 1. History of endoscopic treatments was not dissimilar in the two groups; even if higher in SE group 23/73(32%) versus 22/91 (24%) in NSE group (p=0.41). No intra or postoperative mortality was recorded. There were 7 mucosal lesions: 2 in the SE group and 5 in the NSE group (p=0.45). The median follow-up was 67 months (IQR:24-106). During follow-up 7 patients died, one patient developed a squamous cell esophageal carcinoma in the SE group.
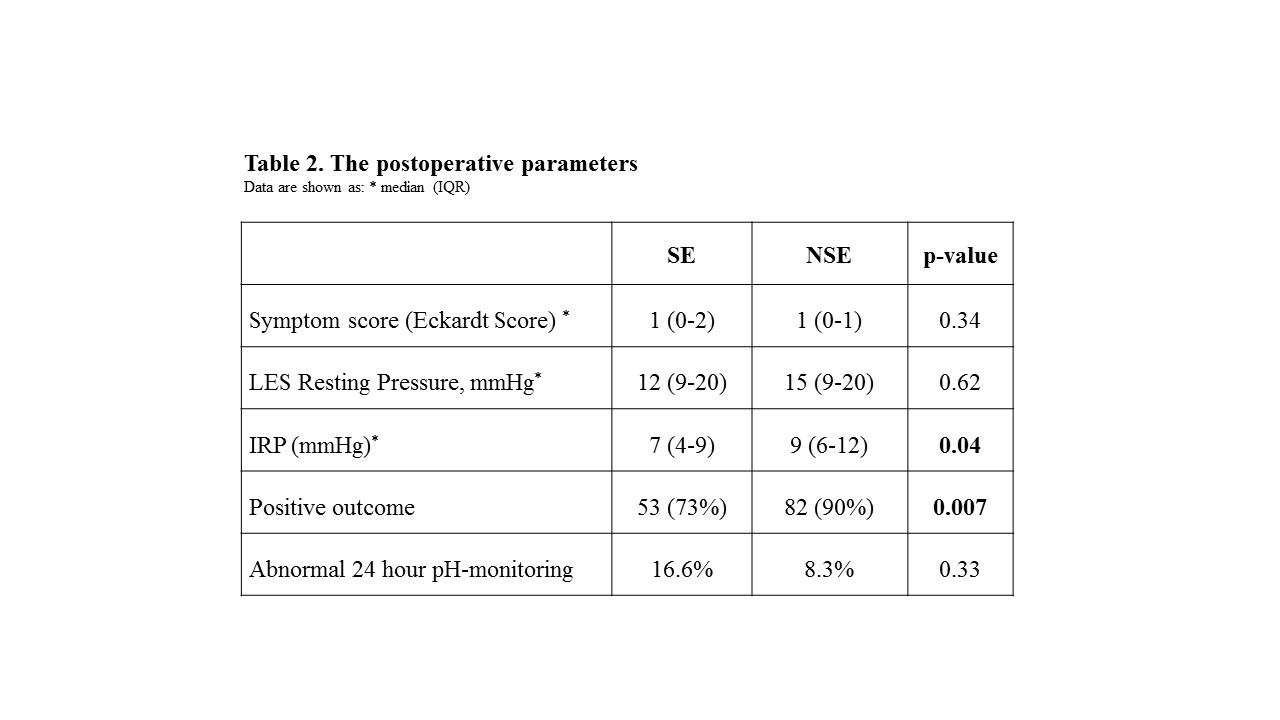
A positive outcome was obtained in 73% of patients in the SE group, as compared to 90% in the NSE group (p=0.007, table 2). Among SE patients, the success rate was lower in patients who underwent a previous endoscopic treatment (12/23, 52%) than in those who did not (41/50, 82%) (p=0.02) while in NSE group, the success rate was not statistically different: 19/22 (86%) in patients who have a previous treatment compared to 62/68 (91%) (p=0.68).
All the patients whose surgery failed subsequently underwent one or more endoscopic pneumatic dilations. The overall success rate of the combination of LHD and endoscopic dilations was 83.6% in the SE group and all patients in the NSE group. The persisting failures had additional treatments: 4 patients a redo-myotomy, one each a botox injection, POEM and only one patient had an esophagectomy; the remaining 5 patients refused additional treatments.
Postoperative 24-hour pH-monitoring was abnormal in 16.6% in SE group and 8.3% in NSE group (p=0.33).
CONCLUSIONS: In end-stage achalasia patients, LHD may still achieve good results by relieving symptoms in more than 70% of patients. Therefore, LHD may still be the first surgical option to be offered to these patients before esophagectomy.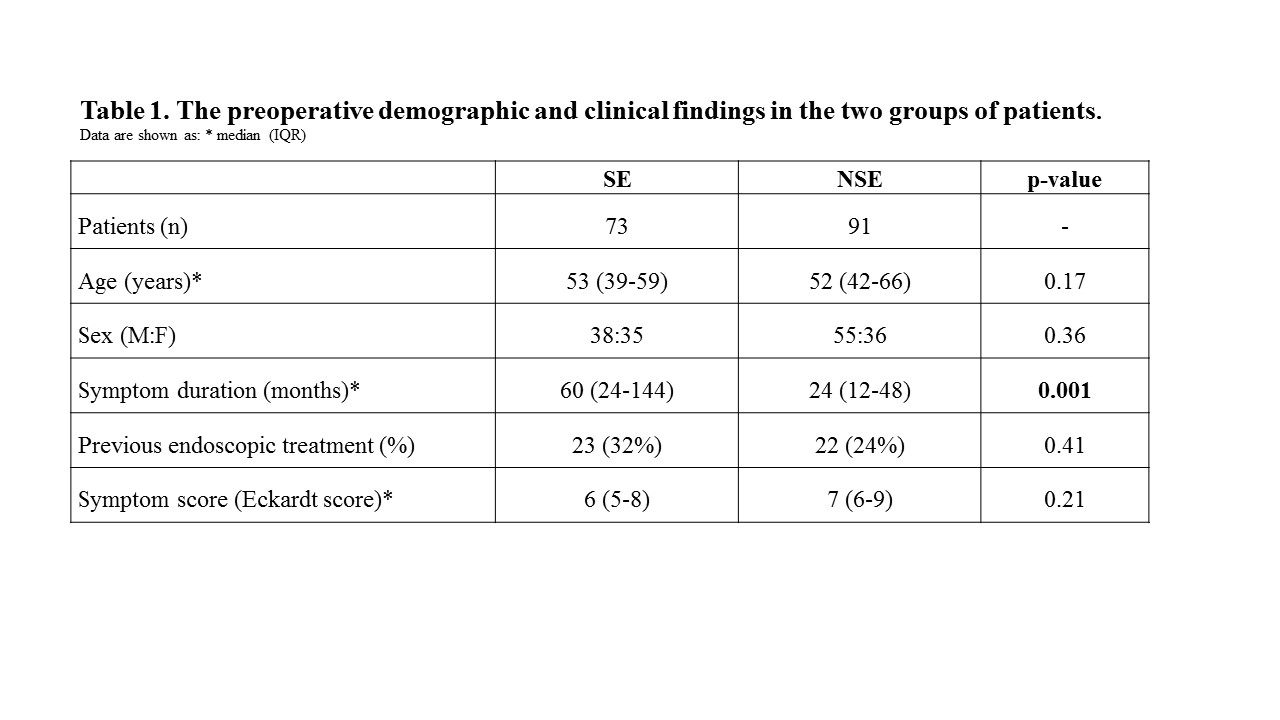
Back to 2021 Abstracts
