ASSOCIATION OF MEDICAID ELIGIBILITY WITH TIMING TO AND OUTCOMES FROM SURGERY FOR DIVERTICULITIS
Adrian Diaz*, Kathryn Taylor, Ushapoorna Nuliyalu, Justin B. Dimick, Hari Nathan
University of Michigan, Ann Arbor, MI
Introduction:
Socially vulnerable patients have been shown to have worse outcomes and greater post-discharge needs. Medicaid dual eligibility has been used as a measure of social risk stratification among Medicare beneficiaries. This study aimed to assess time to surgery, postoperative outcomes, and spending variation by dual eligibility (DE) status among Medicare patients with diverticulitis.
Methods:
Using 100% Medicare claims data, we identified fee-for-service Medicare patients (both DE and non-DE)undergoing colectomy for diverticulitis from 2014-2018. We calculated risk-adjusted, price-standardized payments for the surgical episode from admission through 30 days post discharge and evaluated admission type (i.e., elective vs non-elective), postoperative outcomes, and postacute care (PAC) utilization.
Results:
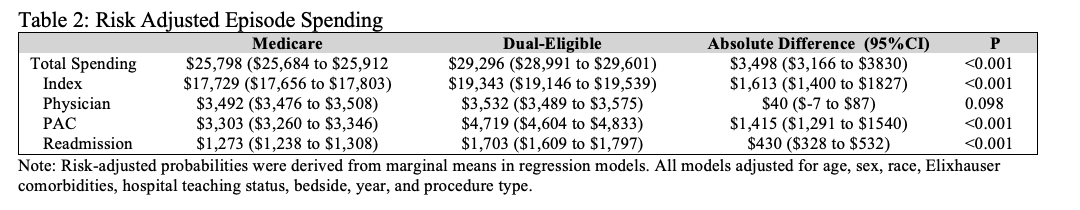
Of the 126,644 Medicare beneficiaries undergoing colectomy for diverticulitis, 17,455(14%) were DE. DE patients had higher odds of having non-elective surgery (OR 1.69 , CI95%1.62-1.76) and higher odds of having an ostomy (OR 1.22, CI95%1.17-1.28). Compared to other Medicare beneficiaries, DE patients had higher odds of experiencing a postoperative complication (OR 1.41, CI95%1.36-1.47), mortality (OR 1.45 , CI95%1.34-1.57), and readmission (OR 1.49, CI95%1.43-1.56). DE patients had lower odds of being discharged home (OR 0.41 CI95%0.40-0.43). Average total episode spending was $3,498 (CI95% $3,166-3,830) greater among DE patients, with the index hospitalization and PAC spending contributing 46% and 40% of the variation, respectively. Even when only comparing patients who had an elective operation and did not receive an ostomy or experience any postoperative complications, DE patients still had lower odds of being discharged home (OR 0.35, CI95%0.33-0.38). Furthermore, the average total episode spending was $1,813 (CI95%$1,582 to $2,044) greater for DE patients with the index hospitalization and PAC spending contributed 43% and 45% of the variation, respectively.
Conclusion
Among Medicare beneficiaries, DE patients were more likely to have a non-elective colectomy and have an ostomy following their operation. Subsequently, DE were more likely to have adverse postoperative outcomes and postacute care utilization, resulting in higher spending. With increasing recognition of the impact of social determinants of health (SDOH) on outcomes and utilization, a patient's DE status may provide an accessible way to identify increased risk attributable to SDOH and intervene prospectively to optimize outcomes and mitigate costs.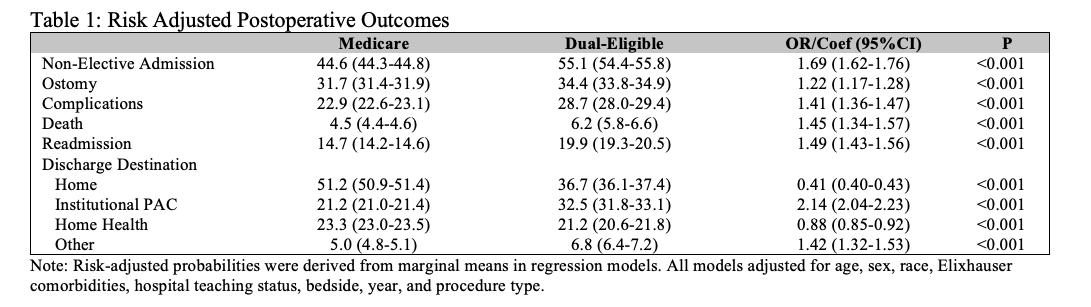
Back to 2021 Abstracts
