DEVELOPMENT OF A NOVEL RISK SCORE TO PREDICT ANASTOMOTIC LEAK AFTER LEFT-SIDED COLECTOMY: CAN WE BETTER DETERMINE WHICH PATIENTS WARRANT DIVERSION?
Nicholas P. McKenna*1, Katherine Bews1, Robert R. Cima2, Cynthia S. Crowson3, Elizabeth B. Habermann1
1Surgery, Mayo Clinic, Rochester, MN; 2Colon and Rectal Surgery, Mayo Clinic, Rochester, MN; 3Health Sciences Research, Mayo Clinic, Rochester, MN
Background: Anastomotic leak (AL) is the most feared complication after left-sided colectomy but is potentially preventable with the use of a diverting ileostomy. However, a diverting ileostomy has its own negative sequelae including an increased risk of dehydration and the requirement of an additional operation for reversal. Consequently, it is critical to accurately assess each patient's risk of AL so that appropriate patients are diverted. This is challenging in practice as many different risk factors for AL have been identified in different single-center studies. Therefore, we used a multicenter database to both develop and validate an AL risk calculator that can assist surgical decision-making on when to divert.
Methods: The American College of Surgeons National Surgical Quality Improvement Program Colectomy Targeted PUF was queried from 2012-2016 for patients undergoing elective left-sided colectomy for cancer, benign neoplasm, or diverticular disease. Multivariable logistic regression identified independent predictors of AL in patients who were not diverted. Point values were assigned to these variables based on their maximum likelihood estimates to develop a risk score. Bootstrapping (200 replications) was performed for internal validation. Visual correspondence between the predicted AL rate and the actual AL rate plus 95% confidence interval was assessed within each risk score decile. Lastly, risk scores were calculated in a separate cohort of patients who were diverted at the time of elective left-sided colectomy.
Results: A total of 38,478 patients (51% female) with a median age of 61 years (range, 18-90) underwent left-sided resection without diversion. The AL rate was 3.3%, and independent risk factors for AL included younger age, male sex, tobacco use, bowel preparation other than combination mechanical and antibiotic, an open approach, and a wound class of III or IV (TABLE). A risk calculator incorporating these variables showed excellent calibration and fair discrimination (raw c-index 0.65, bootstrap validated c-index 0.65) for prediction of AL. Additionally, there was strong visual correspondence with the predicted risk within the 95% confidence interval of actual AL rate for all deciles (FIGURE). Within the cohort of 4,008 patients who underwent elective left-sided colectomy with diversion, the majority (63%) had a calculated risk score decile of six or less, which equates to a predicted AL rate of less than 5% and indicates potential overuse of diversion.
Conclusion: A validated anastomotic leak risk calculator was developed and can be used to stratify patients according to AL risk after elective left-sided colectomy. Intra-operative calculation of scores for individual patients could help guide surgical decision-making for whom diversion is warranted and potentially prevent overutilization of diversion.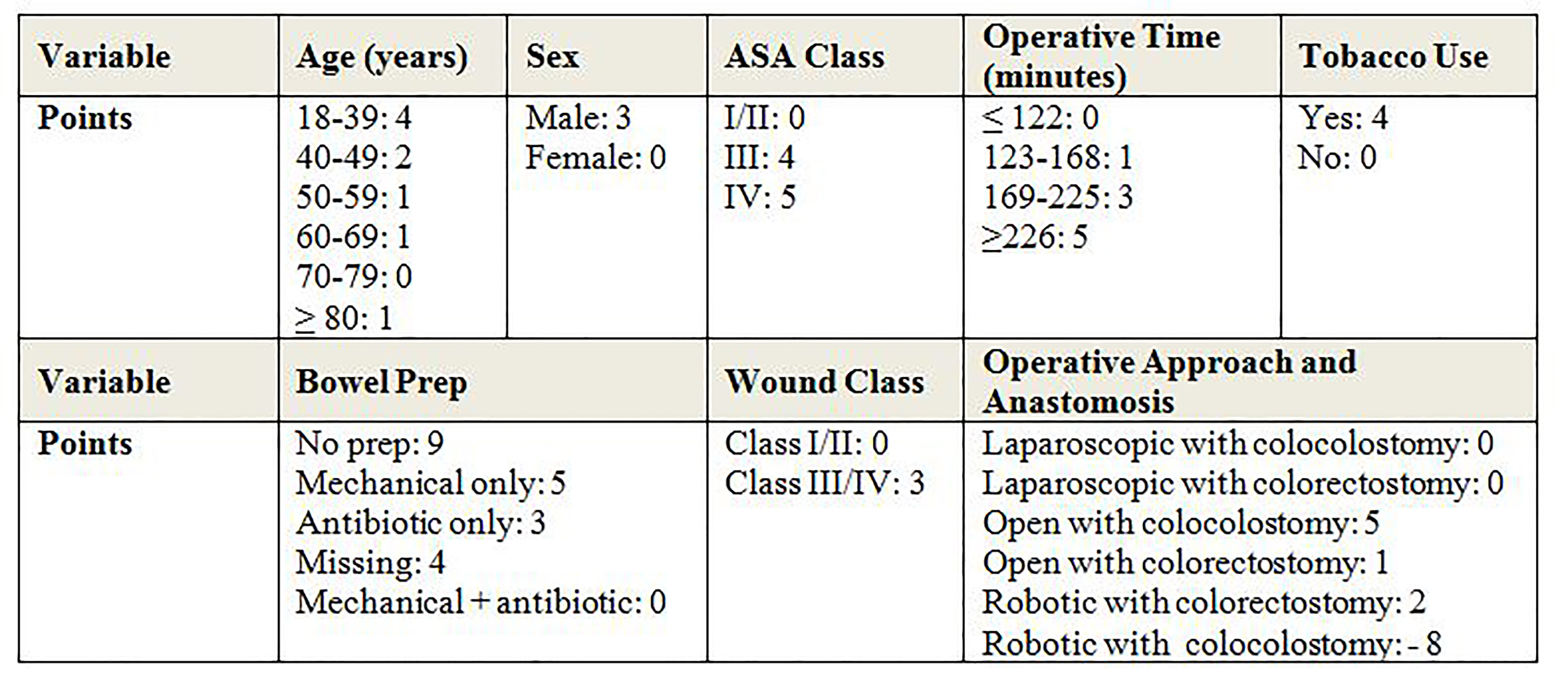
TABLE. Variables include in the final risk score and their relative point values.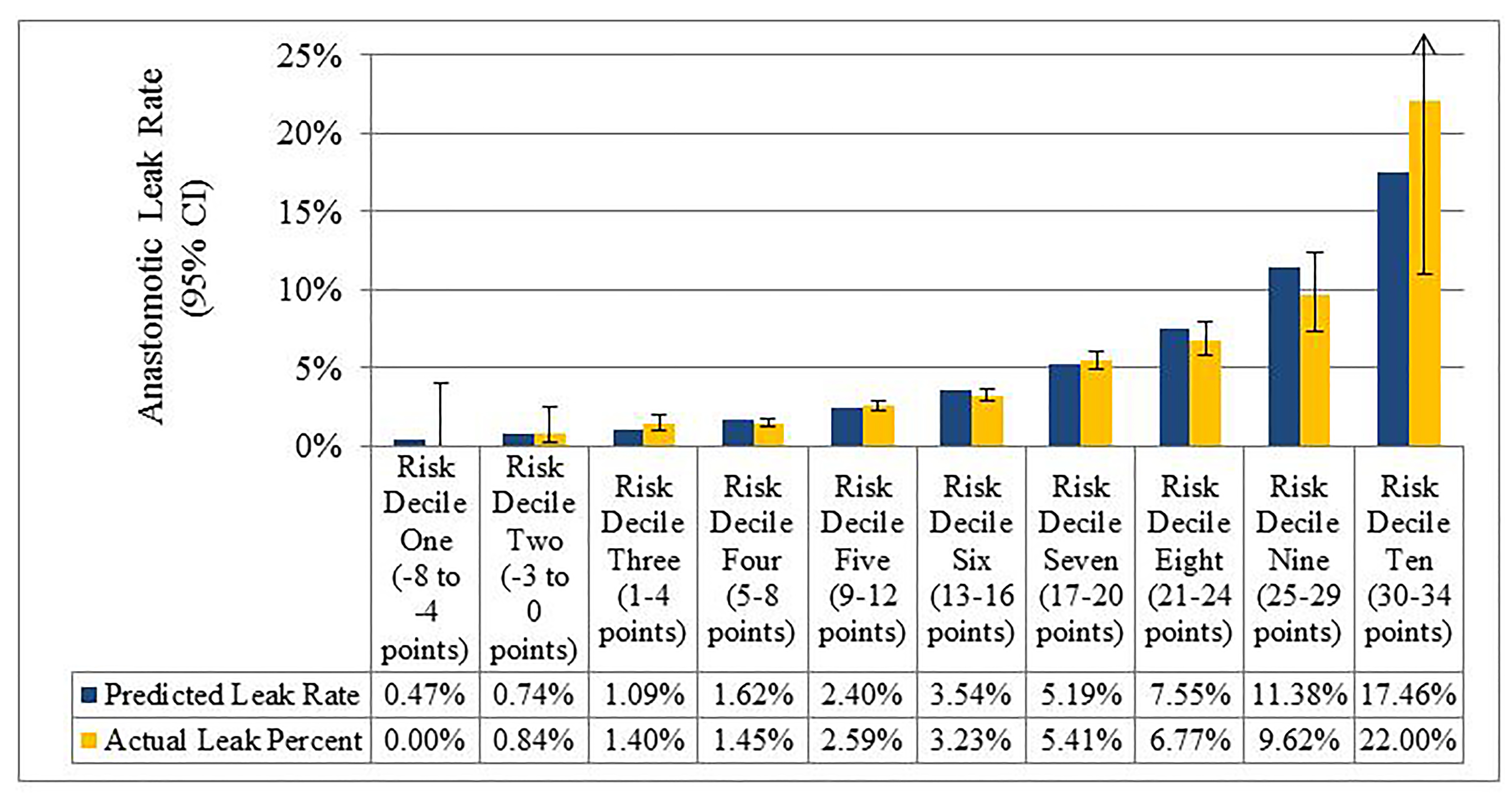
Figure. Comparison between mean model-predicted and observed (95% confidence interval) anastomotic leak rate across the risk score deciles.
Back to 2019 Abstracts




