TRENDS IN COLECTOMY FOR COLORECTAL NEOPLASMS IN ULCERATIVE COLITIS (UC) PATIENTS OVER TWO DECADES: A NATIONAL INPATIENT SAMPLE DATABASE ANALYSIS
Alexander Ni*, Mohammed A. Alqahtani, Maria Aboukhalil, Daniel Marinescu, Carol-Ann Vasilevsky, Nancy Morin, Marylise Boutros, Julio Faria
Colorectal Surgery, McGill University, Montreal, QC, Canada
Introduction: Rates of colectomy for ulcerative colitis (UC) have been decreasing, especially since the introduction of biologics. The impact of reduced colectomy rates on the development of dysplasia and cancer in the chronically treated UC colons is not known.
Objective: This retrospective study was conducted to determine the trend of colectomy for colorectal neoplasms in adult patients with UC over 2 decades, and to identify predictors of colectomy for UC with colorectal neoplasms (UCCRN) in this population.
Methods: After institutional review board exemption, data for adult patients (>18 years-old) with UC were obtained from the National Inpatient Sample from 1993-2015. All total colectomies and/or proctocolectomies were identified using ICD9/10 codes. The primary outcome was colectomy for UCCRN defined as a concurrent ICD 9/10 code for colorectal cancer, rectal cancer or dysplasia/benign colorectal neoplasm. Time trend linear regression and multivariable regression were used.
Results: Of 366,286 admissions with a diagnosis of UC, 16,556 (4.5%) were for a total colectomy or proctocolectomy. Of these, 2,018 (12.2%) had a concurrent diagnosis of colorectal neoplasm, which consisted of colorectal dysplasia/benign neoplasms in 854 (42%), colon cancer in 770 (38.2%) and rectal cancer in 443 (22.0%). The rates of colectomy for UCCRN significantly increased over the study period by 16.3% from 10.3% to 12.3% (pTrend =0.004), while the overall rates of colectomy for UC significantly decreased by 55.6% from 6.3% to 2.8% (pTrend<0.001), representing a significant difference in trends (Time effect=0.310, p<0.001). Among the subtypes of UCCRN, the rates of colectomy for colon cancer remained unchanged (4.5% to 3.9%, pTrend =0.423). However, there were significant increases in colectomies performed for UC with dysplasia/benign neoplasms (by 37.5% from 3.5% to 5.6%, pTrend<0.001) and for rectal cancer (by 36.6% from 2.6% to 4.1%, pTrend =0.028). On multivariable logistic regression, after accounting for age, sex, race, chronic illnesses, long-term steroid use, emergency admission, and post-operative mortality, year of colectomy was a significant predictor (OR 1.035, 95%CI 1.017-1.054) of colectomy for UCCRN.
Conclusion: Despite decreasing rates of colectomy for UC, an increasing number of patients require surgery for colorectal neoplasms. Dysplasia/benign neoplasms represent a higher proportion of cases, suggesting that current screening methods are effective. However, the increased rates of rectal cancer are worrisome and may warrant more frequent surveillance than has been advocated by current guidelines.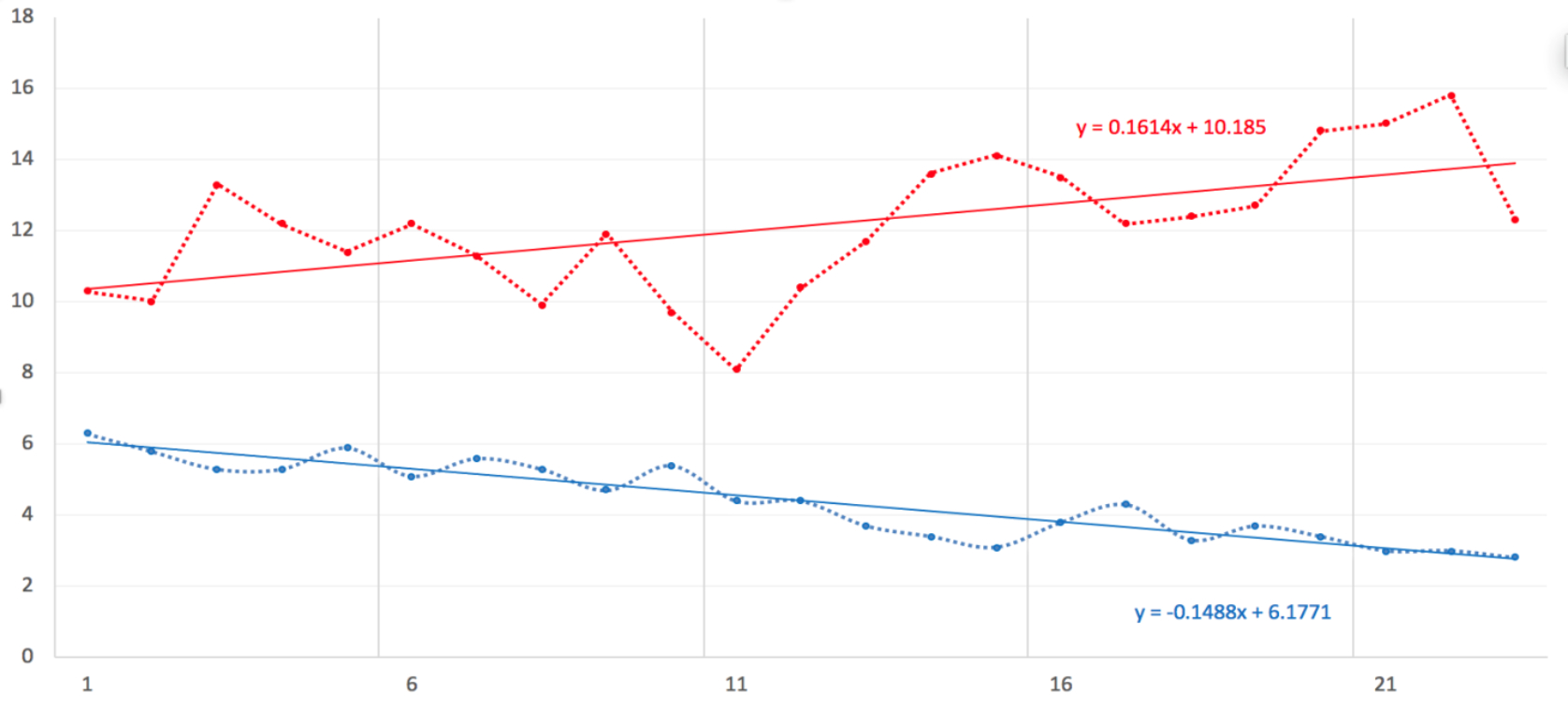
Back to 2019 Abstracts




