|
Back to 2018 Program and Abstracts
HELLER MYOTOMY: DOES ROBOTIC-ASSISTED PROVIDE BENEFIT OVER LAPAROSCOPIC APPROACH? A PROSPECTIVELY CLINICAL DATA BASE REVIEW.
Laura Flores, Priscila R. Armijo, Gurteshwar Rana*, Jake Bianco, Dmitry Oleynikov
University of Nebraska Medical Center, Omaha, NE
Introduction
Heller myotomy is the standard surgical treatment for achalasia. Robotic Heller myotomy procedure rates have increased due to advances in technology and proven safety and efficacy. Despite this increase, evidence of efficacy of this procedure is debated in the literature. The aim of this study was to evaluate symptom improvement in patients who underwent robotic Heller myotomy, compared to traditional laparoscopic Heller myotomy.
Methods
A single institution prospectively collected database was reviewed for patients who underwent either a Robot Assisted (RAH), or Laparoscopic (LH) Heller Myotomy between 2007 and 2016. Only patients who had primary Heller Myotomy followed by a Dor fundoplication were included. Demographics, surgical data and direct cost were analyzed. Frequency of esophageal symptoms and Eckardt score were collected preoperatively (pre-op), and at 6-month (6-mo), 12-month (12-mo), and long term (12-mo+) follow-up. Comparisons were made between LH and RAH. Chi-squared test and ANOVA with post-hoc Tukey tests were used where appropriated. Statistical analysis were performed using SPSS v.23.0, with α=0.05.
Results
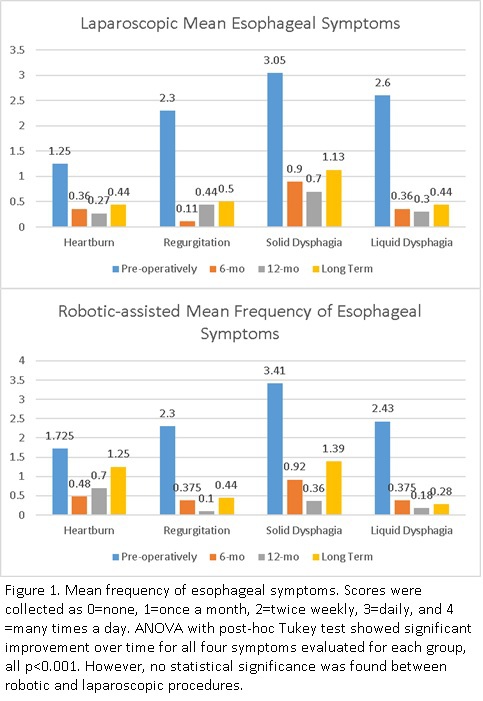
78 patients who underwent Heller Myotomy followed by Dor fundoplication (RAH: N=47; LH: N=31) in this period met the inclusion criteria and were included in the study. Mean age was 55±19.7 and 52±16.4 years for LH and RAH, respectively. Majority of patients were female (LH: 67.7%; RAH: 57.4%) and Caucasian (LH: 83.9%; RAH: 87.2%). RAH and LH were similar in age, gender, race, BMI, preexisting hypertension and diabetes, all p>0.05. One patient in each group had an intraoperative esophageal perforation, which was repaired with a non-eventful postoperative course. Mean follow-up time was 18 months [3-83months] for LH, and 13 months [1-51months] for RAH. There was no statistical difference in the improvement of heartburn (p=.062), regurgitation (p=.856), solid dysphagia (p=.676), liquid dysphagia (p=.988), chest pain (p=.949), or Eckardt Score (p=.857) between groups over time (Figure 1). 1 pt had esophageal perforation each group. Also, use of postoperative PPI was equivalent between groups (LH: 6.4%, RAH: 6.3%), p>.05. Direct cost was also similar between LH ($8,583.42 [$6,548.83-$11,159.04]) and RAH ($9,313.77 [$7,607.30-$10,841.88]) groups, p=.400.
Conclusion
This study demonstrates the comparable efficacy of robotic or laparoscopic Heller Myotomy in esophageal symptom relief for patients with achalasia. Upon comparison between laparoscopic and robotic-assisted Heller Myotomy, we found both procedures to provide equivalent symptoms relieve postoperatively. Cost analysis was also found to be comparable between groups. This conclusion demonstrates that given the comparative results for both approaches, the decision to adopt one versus the other remains surgeon specific.
Back to 2018 Program and Abstracts
|

