
|
 |
Back to 2018 Program and Abstracts
CONCURRENT PPARα AND FXR ACTIVATION MEDIATES NASH IMPROVEMENT AFTER GASTRIC BYPASS SURGERY: A GEO DATASETS ANALYSIS
Guilherme d. Mazzini*3,2, Jad Khoraki3, Mikhail Dozmorov1, Matthew G. Browning1, Richard R. Gurski2, Luke Wolfe3, Guilherme M. Campos3
1Virginia Commonwealth University, Richmond, VA; 2Surgery, Federal University of Rio Grande do Sul, Porto Alegre, Brazil; 3Surgery, Virginia Commonwealth University, Richmond, VA
Background: Weight Loss following Gastric Bypass (RYGB) is associated with significant improvement in Non-Alcoholic Fatty Liver Disease (NAFLD) and Non-Alcoholic Steatohepatitis (NASH), that are better to what is obtained by diet alone. Changes in bile acids (BA) physiology after RYGB have been proposed as mediators for the superior improvements with surgery, through activation of Farnesoid X receptor (FXR) and possibly Peroxisome proliferator-activated receptor α (PPARα). FXR is a major BA target in the liver, and its activation can improve liver lipid, glucose, and energy metabolism; and PPARα stimulates lipid oxidation and inhibits lipogenesis in liver. While in vitro and animals studies have provided evidence that FXR can activate PPARα and FXR and PPARα concurrent stimulation may have a synergic effect on liver fat metabolism, this has not yet been shown in vivo and with clinical correlation. Our aims were to study prevalence and resolution of NASH, and evaluate differences in liver FXR and PPARα gene expression in human subjects at baseline and one year after Diet treatment Alone or RYGB.
Methods: We searched the publicly available Gene Expression Omnibus (GEO DataSets) to identify studies with subjects that had weight loss treatment by Diet Alone or RYGB and paired NASH status and liver genomic data at baseline and follow-up. We identified the study GSE83452 and analyzed its genomic data base to study FXR and PPARα gene expression, on the log_2 scale, from subjects with liver biopsies at baseline and 1-year follow-up, and compared baseline and changes in NASH status and changes in gene expression. Pre-processed gene expression data was obtained using GEOquery R package v. 2.42.0.
Results: Twenty-nine patients had Diet Alone and 25 patients had a RYGB. There was no difference in NASH prevalence at baseline (NASH Baseline: 76% Diet Group vs. 60% RYGB Group, p=ns); the RYGB group had a significantly greater resolution of NASH at 1-year follow-up (NASH 1-year: 59% Diet Group vs. 4% RYGB, Group, p<0.001). Only RYGB group had a significant increase in both PPARα and FXR gene expression (p<0.01, figure 1A). When analyzing only patients without NASH at baseline and follow-up, there was still a significant increase, after RYGB only, in both FXR and PPARα genes expression (RYGB group n=10, Diet Group n=5, p<0.01, figure 1B).
Conclusions: Compared to diet alone, RYGB is associated with an increased rate of NASH improvements and is associated with a greater and concurrent activation of liver FXR and PPARα, even in patients without NASH. Concurrent FXR and PPARα activation fostered by BA changes maybe mediators for the superior rate of NASH improvements of RYGB when compared to lifestyle modification and diet alone.
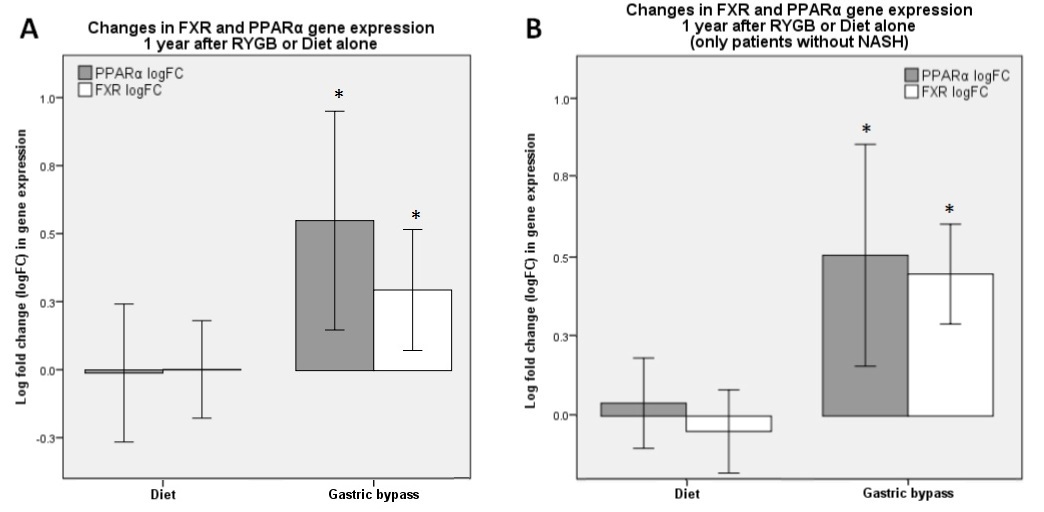
Log fold change (logFC) in liver FXR and PPARα gene expression 1-year after Roux-en-Y gastric bypass (RYGB) or Diet alone. A: All patients with paired samples. B: Only patients without NASH.* P<0.01 compared to Diet group; independent samples T-test.
Back to 2018 Program and Abstracts
|

