Laparoscopic cholecystectomy (LC) has become extensively used in the US; however, reported morbidity varies widely. A reliable method to determine complication risk might be useful to optimize care. In this study, we developed an integer-based risk score to determine the likelihood of major complications following LC.Methods: Using the Nationwide Inpatient Sample 1998-2006, patient-discharges for LC were identified. Previously validated major complications including acute MI, aspiration pneumonia, procedure-related laceration, postoperative infection, DVT, PE, hemorrhage, and reoperation were assessed. Using preoperative covariates including patient demographics, comorbidities, surgical indication, and hospital characteristics, we used logistic regression and bootstrap methods to generate an integer score for predicting in-hospital complication rates. A randomly-selected 80% of cohort was used to create the risk score, with testing in the remaining 20% validation-set.Results: 561,923 patient-discharges were identified with an overall complication rate of 6.5%. Predictive characteristics incorporated in the model included: age, sex, Charlson comorbidity score, surgical indication, hospital type, and admission type. Integer values were assigned, and used to calculate an additive score. 3 groups were assembled to stratify risk, with a 4-fold gradient for in-hospital complications ranging from 3.2 to 13.5%. In both derivation and validation sets, the score discriminated well, with respective c-statistics of .657 and .656.Conclusion: An integer-based risk score can be used to predict complications following LC, and may assist in preoperative risk stratification and patient counseling. These findings may be useful to determine which patients should be referred to specialized centers and/or providers for treatment of gallbladder disease.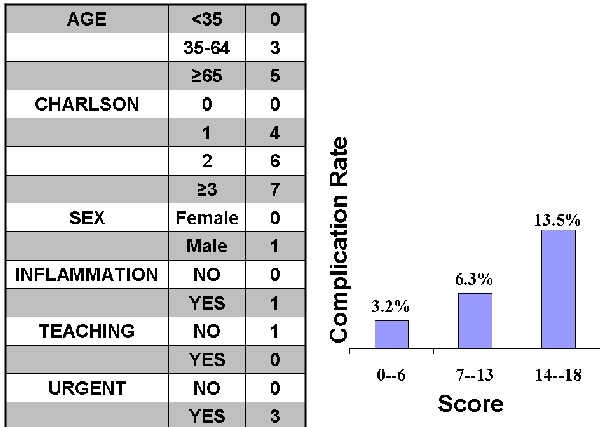
 500 Cummings Center
500 Cummings Center +1 978-927-8330
+1 978-927-8330
 +1 978-524-0461
+1 978-524-0461